Dr.Bill recently published “Hiding in Plain Sight: The impact of non-clinical administrative demand on Canada’s physicians,” our in-depth look into the burdens Canadian physicians face in managing non-clinical work. It’s the first study of its kind to explore this often-overlooked side of doctors’ administrative burden—the behind-the-scenes responsibilities that often come at the expense of time with patients and their own personal well-being.
Among the paper’s most compelling findings is the inequality of results between men and women in the medical industry. Female respondents consistently report higher levels of concern than their male counterparts across key issues such as workload, work-life imbalance, and job satisfaction. As a result, the threat of burnout is significantly higher for women physicians, with potentially serious consequences.
What are the factors driving this disparity? And, more importantly, what can be done to address this inequality toward ensuring fairer, more effective health care for all?
Weighing the burden
The burdens of non-clinical work encompass many demanding administrative tasks—billing, bookkeeping, insurance, and office management, among others—that largely go uncompensated.
These tasks can take up a significant portion of medical professionals’ valuable time, often spilling over from office hours into their home lives. In our survey, one-third of respondents reported devoting over 10 hours weekly to non-clinical work, and 85% said this time typically falls outside of their regular working hours.
Among these results, however, a gender gap emerges, with 91% of female survey respondents saying they spend non-working hours on administrative tasks, compared with 83% of men.
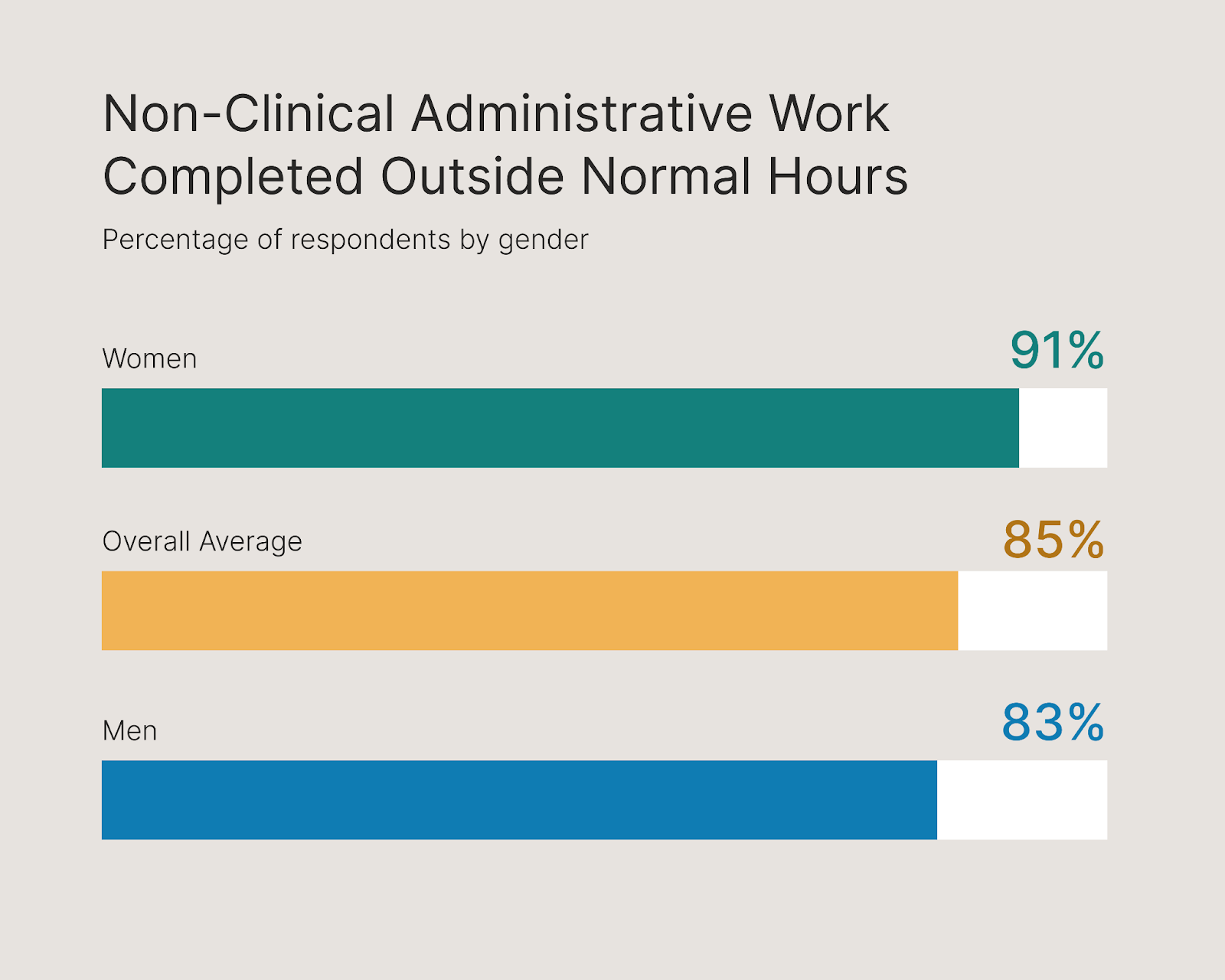
All this added time on administrative tasks not only takes physicians’ time and focus away from their clinical work, but can also have adverse effects on their overall work-life balance. This can take a heavy personal toll, leading to burnout, fatigue, and frustration—and women are disproportionately feeling this burden.
Burnout and dissatisfaction
Recent years have seen more attention paid to the effects of workplace burnout on medical professionals’ health and well-being.
Reports of burnout rates vary, but studies consistently demonstrate the effects are more pronounced among women. A 2021 study published in the Journal of General Internal Medicine found 52% of female physicians reported burnout, compared with 24% of their male counterparts. Other surveys suggest the prevalence of burnout might be as much as 60 per cent higher among women physicians.
In our survey, 72% of physicians overall affirmed that non-clinical administrative tasks significantly contributed to their own workplace exhaustion. Again, a closer look reveals a disparity along gender lines, with 78% of women reporting burnout related to added work, compared with 68% of men.

All these added pressures have a direct effect on overall job satisfaction. While 78% of physicians surveyed affirmed that the volume of non-clinical administrative work has reduced their job satisfaction, this percentage was higher for women (82%) than men (75%).At a time when Canada’s medical workforce faces a recruitment and retention crisis, the rise of burnout across the medical sector is a serious concern, potentially causing patients to miss out on the quality of care they require.
Culture and change
As of 2024, approximately 46% of practicing physicians in Canada are female, and this number is rising, especially among younger doctors and within certain specialties. Despite the many strides made toward workplace fairness, studies like ours show how female medical professionals still face an unequal burden.
For Stephanie Detrinidad, chief operating officer at Dr.Bill, these disparities reflect broader inequality with repercussions beyond just health care. 
“Although it’s great that more women are entering medicine, we aren’t seeing that actually carry through into the profession, with the same representation in leadership roles or academia,” says Detrinidad. “Similar to in any other field, when you look at the CEOs of the major companies and firms, there’s still far fewer women than men.”
Cultural expectations shape women’s experiences at work, and medical professionals are no exception. Studies indicate that while female doctors spend more time on average with patients than do male doctors, they also invest more time in child care, elder care, and other domestic responsibilities.
For Detrinidad, this isn’t surprising. “A lot of women report doing more home-based tasks than their male physician colleagues. They’re more likely to report being a caregiver to a child or a family member or a parent than men, and they’re more likely to report having a spouse that also works.”
Raising a family and taking time off for parental leave can also create specific setbacks for women. In clinician surveys, women more often than men (32.9% versus 19.0%) say child care and caregiving have affected their work. Those who noted this impact in turn reported substantially higher rates of workplace burnout.
As Detrinidad observes, this all adds up to significant challenges for female physicians. “I think all those factors contribute to women having to make different decisions about how they balance career with the unmeasured contributions they have to make with their time.”
Quality care vs. quantity care
The health care industry is known for its long hours and the grueling demands it makes on workers. This grinding aspect has long been accepted as simply part of the job, particularly for professionals early in their careers.
As Detrinidad notes, these demands can force women into tough career choices. “Those intense hours sometimes do overlap with specific times in women’s lives, for example, where you’re in your late 20s or 30s and you’re trying to start a life, maybe a family. You might have to pick your specialty based on lifestyle.”
There are also gender-based variations in the nature of the work itself. Women doctors report having more psychosocially complex patients, fewer resources, and less time for giving patients proper attention than male doctors.
This can all have an effect on the quality of care. “Especially with models like fee-for-service,” says Detrinidad, “you’re not really incentivized to spend more time with your patients. That translates to things like the gender pay disparity, because [doctors] might see fewer patients during the day, but get paid the same amount per visit.”
Bridging the gap
This disproportionate administrative burden can also affect women’s career paths, leading to compensation disparities, lower rates of advancement and academic promotion, and less representation in leadership roles. These discrepancies reflect deeper forces of inequality and bias, both systemically and culturally. Women in health care still contend with frequent gender-related discrimination, microaggressions, and harassment: a 2019 survey by the American Medical Association found that 70% of female physicians experienced some form of gender discrimination during their careers. Such pressures can lead to a hostile work environment, amplifying the already heavy pressures and contributing to the very real risk of burnout.
Looking ahead
What can be done to address, and hopefully remedy, these issues? One practical solution, as Detrinidad suggests, is through adopting new methods for streamlining and optimizing those burdensome administrative processes.
“I often hear doctors say, I didn’t go to school to become a business manager, to learn how to do complicated medical coding. Now there are plenty of solutions that are trying to solve that. That’s why there’s so much interest in AI scribes, for example, because they offload a lot of that work and responsibility to a tool.
“That’s one of the things we try to solve for at Dr.Bill, because we recognize that it takes so much time to do this kind of work. And more often than not, it’s unpaid.”
Other changes might require a more profound shift in established thinking. But that, Detrinidad says, might still be a matter of time.
“Women have only started to really achieve parity in medical school in the last 20 or so years, so there hasn’t been much time for them to reach stages in their careers where they can influence changes in attitudes and policies.
“Maybe that’ll change in the next one to two decades, when the classes that are graduating now progress in their careers. But there are still a lot of older generation doctors working, and that skews the proportion.”
Ultimately, creating a healthier workplace for female medical professionals benefits not only women, but everyone affected by the health care industry: doctors and nurses, support staff, and crucially, patients. Seeking solutions toward easing these added burdens will be critical in ensuring a fairer, stronger, and more sustainable system that works for us all. Download this unique white paper here to explore its full findings. Connect with us to learn how Dr.Bill has taken the pain out of getting paid for more than 20,000 Canadian physicians and counting.
Solutions Designed For The Unique Needs Of Your Practice
Get a $150 Credit when you sign up for Dr.Bill*. No credit card required.




