The OHIP schedule of benefits lists every medical service that doctors are able to bill the Ontario government for. It was last updated on April 1st 2020. Each medical service is given a specific code, with a fixed dollar amount, that the government has agreed to pay the doctor for that service.
The OHIP Schedule of Benefits (often referred to as SOB) is the only list of OHIP insured services that is currently used in Ontario. This means, that although it’s conventionally used under the fee-for-service model, doctors working under an alternative-payment-plan or salary, still need to reference it for reports and shadow billing.
In order to navigate the OHIP schedule of benefits easier, use this mini guide to find exactly what SOB resource you’re looking for:
SOB Resources:
2020 Fee Schedule Code and Premium Changes
The Ontario Schedule of Benefits has been amended to reflect recommendations given by Appropriateness Working Group (the “AWG”).
Haven’t heard of the AWG? The AWG is a physician-led group, which was established back in February 2019 between the Ontario government and the Ontario Medical Association (OMA). Their goal is to use evidence, best practices and expert opinion to improve the quality of patient care and eliminate unnecessary medical services. They do this by recommending changes to the Schedule that will result in shorter wait times and cost savings. The AWG believes that technology and knowledge evolve, and therefore so should the Schedule.
OHIP has released a bulletin that outlines each change. Most of the changes are increases in prices or the removal of certain codes.
Most notably, is the new E084 increase, which will replace the most responsible physician on weekends. This means you’ll get an extra 45% when for subsequent visits and C122, C123, C124, C142, C143, C882 or C982-add.
This replaces E083 (on weekends), which was an extra of only 30%. However, from Monday to Friday would still use E083.
The OHIP Schedule of Benefits 2020
The schedule of benefits is a 960 page PDF that lists around 6,000 services, covering every specialty and includes premiums, rules and descriptions. This makes finding the right fee code time-consuming and tedious.
For easy searching, we suggest book marking the online OHIP searchable database.
This is a digitized list of all the OHIP fee codes that are currently available in the SOB. Each code includes a description along with the billing rules, and the dollar amount.
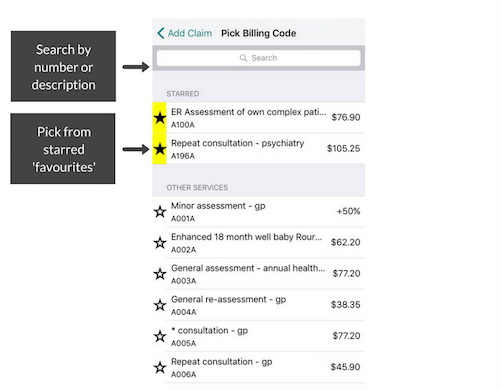
You can search by specialty, billing code or keyword, so you can quickly reference and find what you’re looking for. This is especially beneficial when you’re billing on the go or in a busy work setting.
The General Preamble
The General Preamble provides the rules, guidelines and billing requirements under which the fee codes are to be claimed. These rules were established to help clarify the schedule of benefits and make it easier to understand.
If you’re new to billing in Ontario we suggest reading over the General Preamble at least once. This will help you better understand the SOB terminology.
The General Preamble starts on page 1 and goes until page 124 (see below).
The first section provides definitions for the terminology used throughout the schedule of benefits. For example, age definitions, time definitions, descriptions of maximums, minimums and time/unit-based services.
When you’re reading the SOB, if a word is italicized it means the definition for that word is found under the Definitions Section.
Following ‘definitions’ is general information and rules. This section is the
foundations of the OHIP schedule of benefits. It relates to medical records, modifications, payment rules, assessment rules and the use of prefixes and suffixes.
For example, for surgical codes, suffixes are required to identify:
-
If the physician performs the procedure (Suffix A).
-
If the physician assisted at the surgery (Suffix B).
-
If the physician administered the anaesthetic (Suffix B).
The next 16 sub-headings of the General Preamble continue to outline the different rules and services for different areas of care; such as: assessments, consultations, counselling services, interviews, delegated procedures, premiums, surgical assistant services, anesthesiologist services, and emergency department fees and agreements.
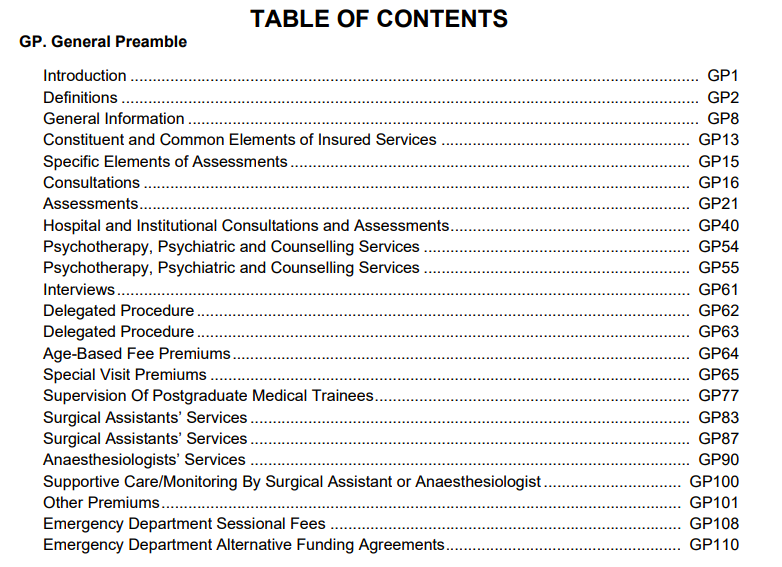
After the general preamble, the schedule of benefits outlines the list of fee codes, along with their descriptions and the dollar amount.
The OHIP schedule of Benefits PDF: 2020
Fair Warning: Reading the schedule of benefits isn’t easy (or generally enjoyable). However, understanding what codes are available within your specialty is a great way to optimize your billing.
To help you get started, we’ve compiled the most common billing codes per specialty and listed them below.
So, grab a coffee, read them over and start getting familiar with what’s billable today!
What’s more? We’ve also put together OHIP’s most common Surgical Procedures and Diagnostic & Therapeutic Procedures.
Tip: Once you’re familiar with what’s available to your specialty, create a billing cheat sheet of frequently or most commonly used billing codes.
Otherwise, just bookmark the appropriate pages below in your web browser for easy searching.
The Most Common OHIP Billing Codes by Specialty
Physical medicine & rehabilitation
Family practice & practice in general
Internal and occupational medicine
The Most Common OHIP Surgical Procedures
Urogenital and urinary surgical procedures
Male genital surgical procedures
Female genital surgical procedures
Neurological surgical procedures
Ocular and aural surgical procedures
Integumentary system surgical procedures
Musculoskeletal system surgical procedures
Respiratory surgical procedures
Cardiovascular surgical procedures
Haematic and lymphatic surgical procedures
Digestive system surgical procedures
The Most Common OHIP Diagnostic & Therapeutic Procedures
Nerve blocks for acute pain management
Nerve blocks – interventional pain injections
Nerve blocks – peripheral/other inections
Psychiatry and respiratory disease
Looking for More Billing Resources? Check out our Ultimate OHIP Billing Guide and learn how to maximize your claims and save time.
SOB Diagnostic Codes
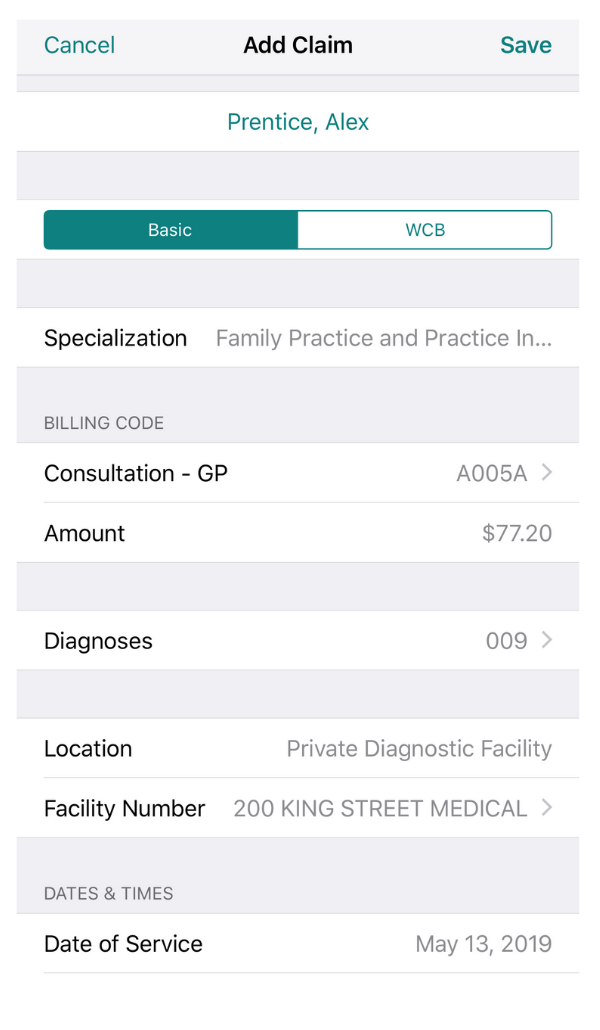

If you’re using the schedule of benefits to submit claims to OHIP, remember that every claim you submit MUST HAVE a diagnosis code along with the billing code.
For example, in the following picture, the fee code is A005 (Consultation). The diagnosis code selected is 009, which stands for diarrhea.
Is you’re looking for a specific diagnostic code, scroll through OHIP’s diagnostic resource manual.
(If you’re using Dr. Bill just search on the app by keyword).
OHIP Remittance Advice (RA) Reports
Each month OHIP will send a monthly remittance advice (RA) Report and a Claim Error Report. These reports let you know, in detail, which claims have been approved, paid with adjustment, rejected or have errors that you need to fix.
-
Submission Error Codes
If you get a submission error then your claim didn’t pass OHIP’s pre-edit approval process.
This isn’t a big deal, it just means you’ve made a mistake when submitting your claim and didn’t follow one of the rules outlined in the OHIP schedule of benefits.
While this will delay your payment, submission errors are usually easy to fix.
Most errors are a direct result of:
-
The wrong use of SLI code
-
There’s a fee code conflict – so assessment is required
-
Invalid use of OHIP Premiums
-
No Referring Physician
-
The Patient doesn’t have insurance
If you do get a submission error it will be outlined in your Claim Error Report using a specific code. This code explains what SOB rule you violated.
To fix the mistake, use our search tool to find the code from your Claims Error Report, so you can figure out how you can fix and resubmit it.
-
Rejections
Sometimes, your claims might be rejected or paid at a reduced amount. When a claim does get rejected or is reduced, you can resubmit the claim and inquire to appeal the decision.
To inquire about your rejected claims you need to fill out the Remittance Advice Inquiry form.
This needs to be done within four months from the issue date of the RA report (that detailed the claim in question).
Also keep in mind that claims have to be submitted within six months of the original date of service. Anything submitted after six months will be rejected and become ‘stale dated‘ claims.
***If you are billing with Dr. Bill, most of our plans offer rejection management. This means our billing agents will automatically handle and resubmit all your rejections and submission errors for you.
How OHIP fee codes are Priced
The dollar amount of each fee code outlined in the OHIP schedule of benefits is negotiated between the Ontario Ministry of Health and Long-Term Care and the Ontario Medical Association (OMA).
Both sides go through every fee code to determine how much the prices should be, based on how long the service or procedure takes, as well as the complexity involved. Helping in the SOB decision-making process are elected doctors who represent a specific region and specialty.
Since technology is always changing, especially in the medical world, certain services and procedures become less complicated, and thus fee codes are often lowered.
Likewise, sometimes fee codes are evaluated and determined that they are too low and thus the dollar amount increases. The OHIP schedule of benefits is constantly being revised and updated so that each fee code properly reflects the current realities of the service.
The OHIP Schedule of Benefits Updates
While the schedule of benefits is only updated every 4 years, you can find current amendments and changes released frequently in the OHIP Bulletins.
Tip: Make sure the software system you’re billing with has automatic SOB updates. That way, anytime the schedule of benefits gets updated, the billing codes you’re using will be current and correct.
If you can’t get updates automatically, then just make sure you bookmark the OHIP Bulletins and check back with it regularly.
If you’re billing with Dr. Bill, when OHIP releases new fee codes, or adjustments, they are automatically updated and available both on the app and the web version.

The OHIP schedule of benefits can be confusing, inconsistent and it doesn’t always provide clear answers.
If you ever have a question about a rule, premium or fee code contact one of our OHIP billing experts today. They know the SOB rules like the back of their hand, and can help you sort through anything!
This article offers general information only and is not intended as legal, financial or other professional advice. A professional advisor should be consulted regarding your specific situation. While information presented is believed to be factual and current, its accuracy is not guaranteed and it should not be regarded as a complete analysis of the subjects discussed. All expressions of opinion reflect the judgment of the author(s) as of the date of publication and are subject to change. No endorsement of any third parties or their advice, opinions, information, products or services is expressly given or implied by RBC Ventures Inc. or its affiliates.
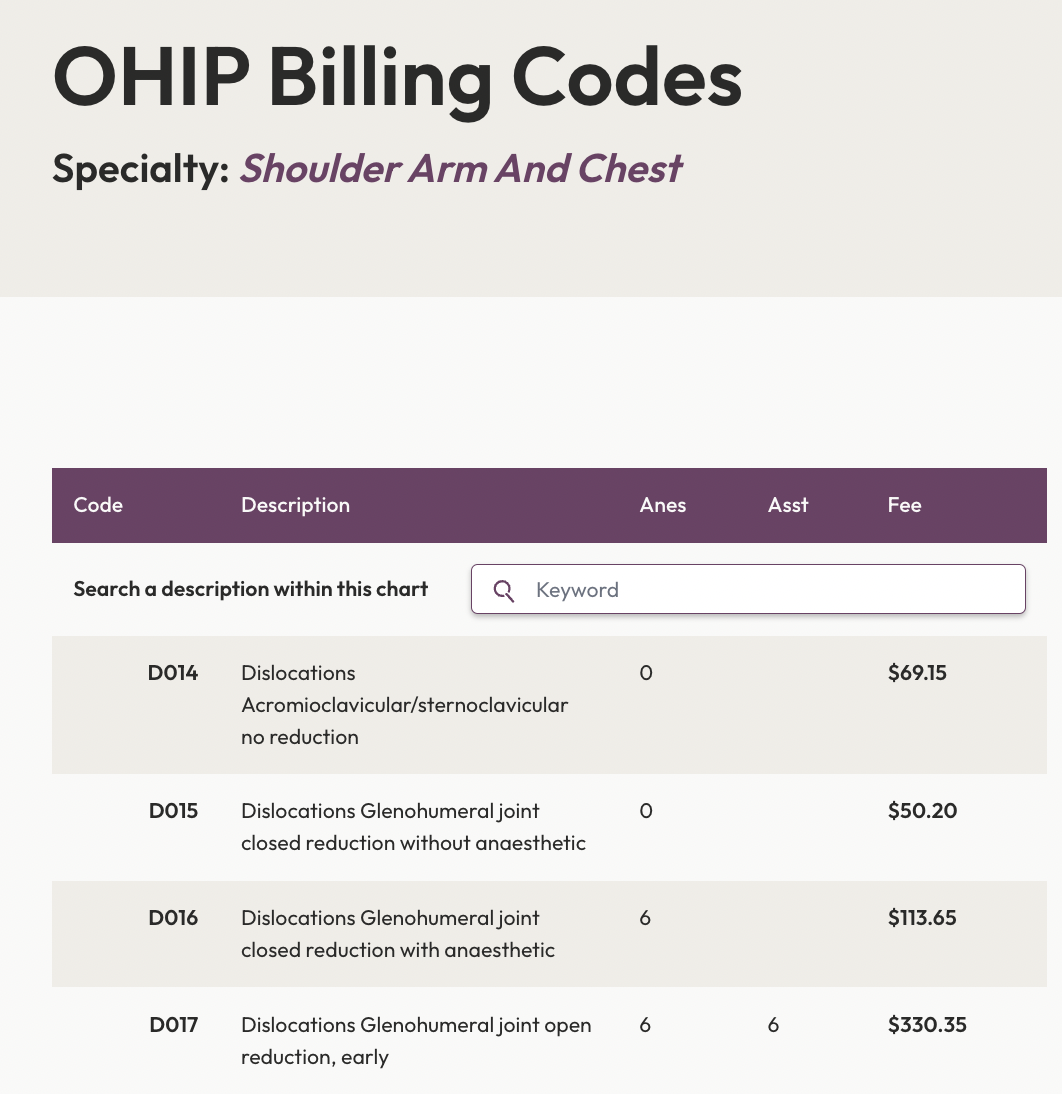
Search All OHIP Billing Codes
Search the Ontario Schedule of Medical Benefits electronically. We’ve digitized all the OHIP billing codes so you can easily find the most up to date billing rules and amounts.