Once a month OHIP will send you two reports – a summary of all payments you’ll receive, and a listing of any unprocessed claims or refusals that they didn’t approve. These reports are not only helpful for bookkeeping but are essential for keeping track of any claims you submitted during the last month. It’s a good idea to get into the habit of reviewing these reports so you can make sure you’re getting paid correctly. Here’s a deeper look into your OHIP Remittance:
Remittance Advice (RA) Report
The RA report is a listing of all of the claims you made that were approved or paid with adjustment. You’ll get this report around the beginning of each month – typically between the 1st and 7th. You can expect the payout for these claims around the 18th of each month. Since OHIP claim submissions run on a monthly cycle, any claims you submit up until the 18th of each month will be processed for payment by the 15th of the next month. Claims received after the 18th of the month probably won’t be processed in time before the next remittance, therefore you should always submit any pending claims before 12pm on the cut-off date (so that they’ll show up on your remittance/next payment).
How your OHIP RA report will look depends on who is submitting your claims for you (a.k.a. your billing service). Scroll down to the ‘ Active Claims Status’ section of this page to see an example of how an RA report might look.
Claims Error Report
The second report you get from OHIP is a claims error report – this is a listing of all the claims you have submitted that have come back with errors, such as using the wrong code, submitting a claim you’ve already submitted, or choosing an invalid specialty. Again, this report will look different depending on who is submitting the claim for you, regardless it’s important for you to review it.
If OHIP rejects or adjusts a claim, the corresponding error code will appear on the report, letting you know the reason for the refusal. You can use our searchable database to find the error code from your report and follow up on any claims you might need to resubmit or clarify with OHIP.
Remember there’s a difference between a refusal and a rejection. A refusal means your claim has a simple error (one that you can fix and resubmit quickly like a mistake in your patient’s name or you forgot to add a referring physician). A rejected claim means your claim has ‘gone against’ a billing rule – these take longer to fix and aren’t guaranteed approval.
Reconciliation and Payment
When a claim does get rejected or the payment is reduced, you can try to resubmit the claim in hopes to appeal the decision. To do this you need to submit the Remittance Advice Inquiry form. This needs to be done within four months from the issue date of the RA report that detailed the claim in questions. Keep in mind that claims have to be submitted within six months of the original date of service. Any billings submitted after that deadline will be rejected and become ‘stale dated‘ claims.
The process of reconciliation is time-consuming and confusing. If you find your getting a lot of refusals and rejections we suggest making sure your billing software offers rejection management – that way expert billing agents can go in and resubmit any rejections you may have for you (If you’re looking for an affordable service Dr.Bill has a 97% payout rate of resubmitted claims)!
Active Claims Status + OHIP Remittance Advice (RA) Report
When you bill through Dr.Bill, you have the option of seeing the current status of all of your active claims on your claim dashboard. Your claim dashboard will allow you to see the status of each claim, a list of refusals, a list of rejected claims, and which of your claims have been paid, with or without adjustment. This is different than the traditional RA reporting because you’ll be able to track everything – not only already paid claims.
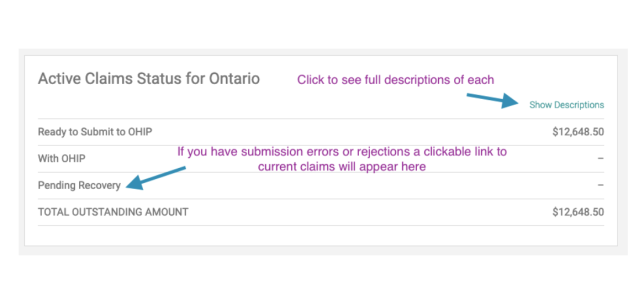
Once you log in, your dashboard will display the current status of all of your active claims.
- Click on “Show Descriptions” to display a drop down menu of what each status means (this will bring you to the second photo)
- Click on “Submission Error” to see a list of current refusals.
- Click on “Rejected” to see a list of rejections.
***Important Reminder: The dashboard page is live so numbers here will always change depending on whether claims are being resubmitted or released.
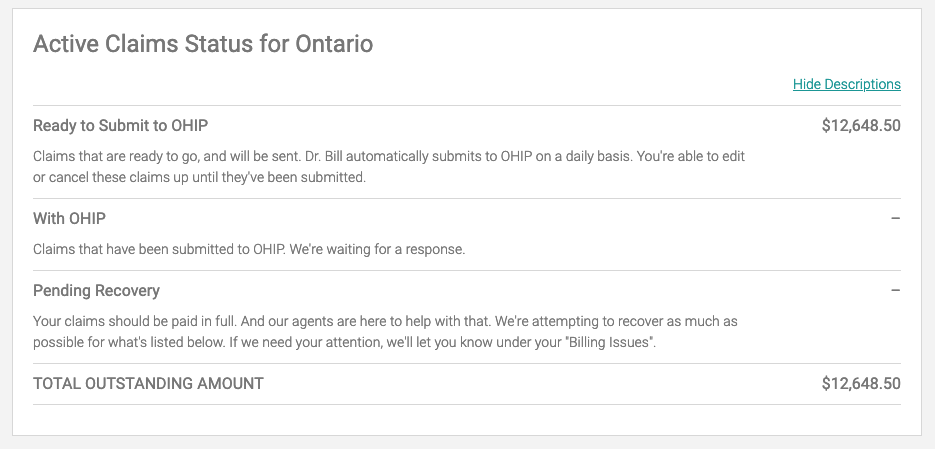
Note: If you’re on the self-serve plan, “Pending Recovery” will display “Unresolved Claim Amounts.” By Clicking on “Show Description” it will display the descriptions of your active claims. The display will look like this:
OHIP Remittance Report Payment Breakdown
If you’re looking for a payment breakdown, or to find out more information on a specific payment period or claim, follow these steps:
- From the dashboard click on “Reports”
- Then click on “Payments.”
- Put in the dates you’re interested in and click “search.”
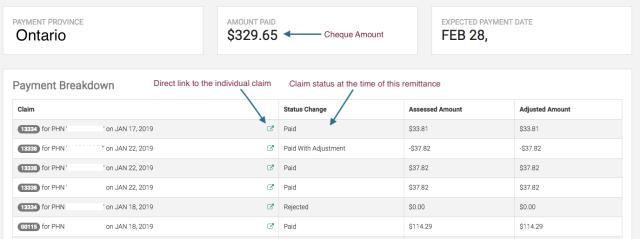
A payment report will be displayed for your chosen dates, giving you a breakdown of each claim and the status of the claim at the time of the last payment report.
By clicking on the claim you’ll get a complete overview of it.
On this dashboard, you can see each of your active claims, the amount they were assessed for, and any adjustments made to the amount billed. It will tell you what the claim’s status is at the time of the remittance as well as provide a direct link to the claim in case you’re looking for more details. And while it might seem time consuming to go through every single claim for the month, taking a look at this report is a good idea so you can keep track of exactly how much you’re getting paid. This reporting tool is some of our users most treasured feature:
“”So convenient and I love the instant feedback at the end of the day that tells me how much I’ve billed. The homepage that reports the status of total billings is also very clear. My billing…what’s been paid/held/refused was always very vague with my prior billing service. I also never really had a good idea of how much was outstanding and was submitted for a given billing cycle. I’d eventually get some information but usually 2 or 3 months later.”
Dr. Val Montessori
{__}
“It is far superior to the previous billing tool I was using – in particular the reporting features”
Dr. Dan Lin
Psychiatry
“Dr.Bill’s platform is very easy to use and very transparent. I can see what’s
rejected, what’s submitted and what’s pending very easily. I can’t do that with
any other platform.”
Dr. Maria Wu
Obstetrics and Gynaecology
If you have any questions in regards to claims, reports or Remittance Payments, please don’t hesitate to contact our billing team.
This article offers general information only and is not intended as legal, financial or other professional advice. A professional advisor should be consulted regarding your specific situation. While information presented is believed to be factual and current, its accuracy is not guaranteed and it should not be regarded as a complete analysis of the subjects discussed. All expressions of opinion reflect the judgment of the author(s) as of the date of publication and are subject to change. No endorsement of any third parties or their advice, opinions, information, products or services is expressly given or implied by RBC Ventures Inc. or its affiliates.