This is a condensed mini-guide on MSP billing for general internal medicine (GIM) practitioners. For a downloadable version scroll to the bottom.
Consultations
MSP states that all new consultations require a written letter from the referring physician and that you (the attending) provide a written report on your findings to the referring physician within 2 weeks. In practice this isn’t used for day-to-day billing, but your documentation would be required if you were to be audited.
You can bill a new consultation on a patient if a new condition arises during their stay. If you’ve already billed a new consult and a new condition arises you should bill a 00310. However, if your patient meets the criteria for complex conditions, you can bill a 00311 (3 new conditions). A 32212 (1 new condition) if you are approved to bill GIM fee codes, or 00312 (1 new condition) as the unrestricted equivalent.
00310 – New Consultation
Only paid once per 6 months, per diagnosis. That’s across all physicians, so if another physician logged a New Consult (same billing code) for the same diagnosis (ICD9 code) in that 6 month interval you can’t bill for it. Of course, you’ll likely not know if this is the case, so it’ll get rejected and we’ll re-submit as a Limited Consult.
If the patient develops a new condition/diagnosis within that 6 month interval you can log a new consultation. MSP matches the billing code to the ICD9 code logged on the claim to determine if it is valid.
00312 – Repeat or Limited Consult
Log this when you’re requested to do a consultation but a New Consultation has already been logged for that diagnosis in the past 6 months. Also logged if the Consult isn’t as comprehensive as a Full Consultation and it doesn’t warrant the full fee (ex: it’s less effort).
There’s no specific written timing rule for how often you can log a Limited Consult, however in our experience it’ll get rejected if another Limited Consult has been logged within the previous 42 days. It’s expected that a Limited Consult is logged as part of Continuing Care for a patient, but it must be requested.
00311 – Complex Consult (3 Conditions)
Paid once per patient, per hospital admission/visit and doesn’t have the 6 month requirement of a 00310. Patient must have 3 of the listed medical conditions (we provide that ICD9 list when you select the code). Or in some circumstances, have only 2 conditions from the list and a third not on the list. In this case you must provide an explanation (in the Notes) of the medical necessity for the Complex fee code.
32212 – Repeat or limited consultation
You can bill this when a consultation for same illness is repeated within six months of the last visit, or if in your judgment the consultative services doesn’t seem appropriate for a full consultative fee.
Continuing Care
32308 – Subsequent Hospital Visit (2 or 3 Conditions)
Requires that a 00311 has been logged on the patient in the past 6 months. You can only log these claims for the first 10 days of hospitalization, thereafter you need to log a 00308. Our app prompts you when the 10 day period is up (provided the admission date was available on the label or it was entered by you when you added the patient).
32208 – Subsequent Hospital Visit (only available if you’ve completed 3 years of core Internal Medicine training plus at least 1 year of General Internal Medicine training.
For this one, you don’t have to bill 00311 beforehand. It can be billed all on its own and you can bill for it multiple times in a day if there’s a medical necessity. Just indicate that in the notes.
32307 – Sub Office Visit (2 or 3 Conditions)
Payable only if a 00311 has been logged in the past 6 months.
00306 – Directive Care
You can only bill this twice per calendar week (Sunday to Saturday), and it’s only billable if the responsibility for the case remains in the hands of the of the attending practitioner but you, as the referring physician, request a consult to give directive care in hospital during the acute phase.
This means that you bill 00306 when you’re not the MRP for the patient and only see them twice a week. If you’re the attending practitioner you’d bill 00308 (see below).
00308 Subsequent Hospital Visit
You can bill this code multiple times in a day if required, but you’ll need to provide an explanation in the notes as to why the patient needed to be seen more than the initial visit. After 30 days you can only bill this twice per week, unless you provide an explanation in the notes why the patient required the additional visits.
00305 Emergency Visit
If you’re called out after hours to urgently see your patient (whether as the attending or referring) physician you can bill 00305.
These claims require a start & end time (our app will ask you to provide these), however, you cannot bill a Call Out or Continuing Care premium (see below for more on these fees).
Call Out & Continuing Care
You get paid a premium on top of your consultations/procedure fees anytime you’re specially called out to render servicesafter 6:00pm (weekdays) or on Weekends. You don’t have to be at home when you’re called, just not in the hospital.
This doesn’t apply if you’re scheduled for weekend or evening service as part of your hospital coverage. So if you’re working on the weekend, and saw patients you can’t bill these. However, if you went home and were on call that evening and had to go back you can.
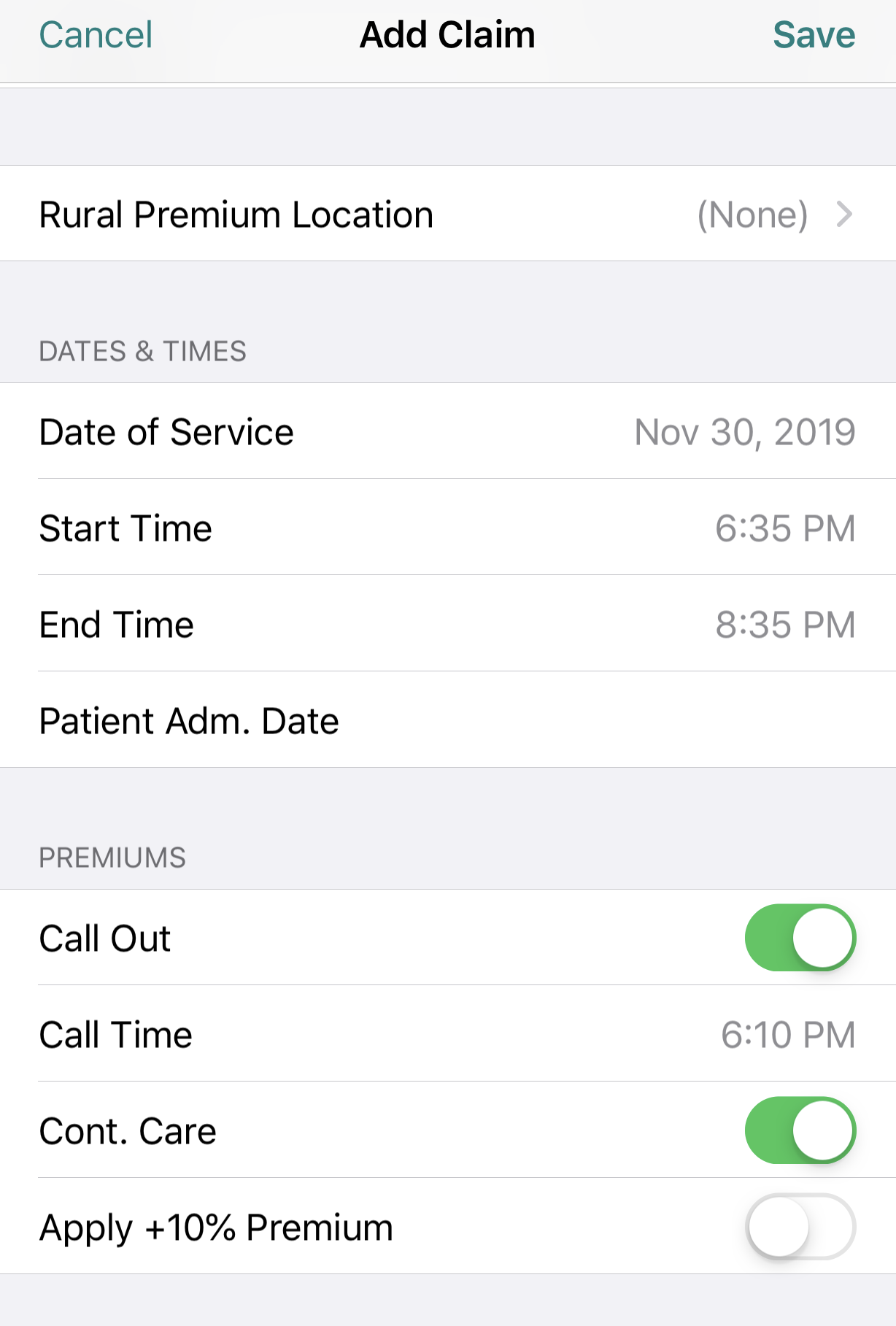
On Dr.Bill you can log these premiums by toggling the Call Out and Continuing Care buttons on your app. Enter your Call, Start & End times and the amount will get added to the base fee for your consultation.
Guidelines
For the first patient you see when called out, toggle both ‘Call Out’ and ‘Continuing Care’. If you see any subsequent patients while at the hospital on that call, toggle just Continuing Care and you’ll get paid for each 30 minute interval you spend with each subsequent patient.
If you saw patients for less than 15 minutes each, add up the total time and log that against the last patient you saw. Ex: If you saw 3 subsequent patients after the first call for 10 minutes each, toggle the After Hours button for the last patient and log a 30 minute interval and indicate in the notes you saw 3 patients for 10 minutes each).
Medical billing in BC is confusing and can often be overwhelming. To help out, check out our complete MSP guide that walks you through each step of medical billing – from the general teleplan process to maximizing your claims and using mobile billing.
Other Fees
Here’s some other fees that are commonly billed by other GIM specialists.
10001 – Telephone Call Specialist Advice
You can log this when you are called for a consultation/advice on a patient over the phone. You can’t log this when you initiate the call nor can you add Call Out or Continuing Care premiums to the claim. This is not payable for booking an appointment, arranging a consultation or procedure, lab results, etc. Only for discussion about the care of the patient. The call/conversion should be noted in the patient’s chart (auditing purposes).
78717 – Specialist Discharge Care Plan for Complex Patients
Billed for patients who require community support upon discharge and are otherwise at risk of readmission. A detailed care plan must be created for the patient. Patient must have been admitted for 5 days or longer, not application for elective procedures, care plan must be included in the patient’s medical record. You must be the MRP for this patient.
You cannot bill this with any ‘out-of office premiums’ or 10004.
78720 Specialist Advance Care Planning Discussion Extra
You can bill this if you have a discussion with the patient and/or their family about future care of a patient as their health deteriorates. However, you cannot bill this fee code for critical care patients.
A care plan template must be filled out with the consultation.
00314 Internal Medicine Prolonged Visit for Counselling
MSP defines counselling as the discussion with your patient, caregiver, spouse or relative about a medical condition, in which you recognize as difficult, or where you notice the patient is having significant emotional distress, including the management of malignant disease.
To claim 00314 it must not be delegated and last at least 20 minutes. You can bill this 4 times a year, per patient.
10003 Specialist Telephone Patient Management Follow-up
You can bill this if you have a phone call with the patient to discuss their care or condition. You have to have seen the patient previously in the past 18 months and you cannot bill for this if you billed for other claims on this patient for the same day.
If you’re interested in other MSP fee codes, make sure to save a link to our MSP billing codes searchable database. You can search by speciality, billing code or keyword.
MSP Billing Code Lookup
Final Takeaway:
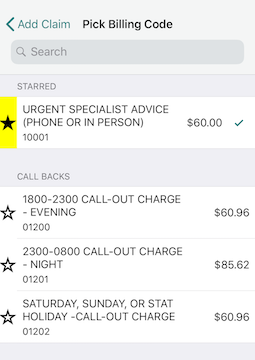
Remember you have the option of ” starring” your most commonly used billing codes. That way, they’ll appear at the top for searching.
If you have any questions about GIM codes or would simply like to clarify something, don’t hesitate to get in touch with us.






