It’s nice to get paid on time and to know you’re being paid properly for all the work that you do. Unfortunately, when it comes to medical billing, this isn’t always the case. Everything you submit doesn’t always get approved and the rules for certain MSP fee codes aren’t always clear. It’s normal that you’ll slip up from time to time and get a few rejections or miss out on a few premiums.
Luckily, with modern improvements in medical billing software, submitting claims to MSP is still much easier than it used to be. That being said, over the past year we’ve seen a number of common mistakes when it comes to MSP rejections, along with a couple of things you might be missing out on. Below we’ve listed 10 MSP billing tips to help you reduce rejections and optimize your claims.
1. Call Out & Continuing Care Premiums
If you’re called out to the hospital on an urgent, non-elective basis you can bill a Call Out (01200, 01201, 01202).
During weekdays the call must be placed prior to 8am or after 6pm. On weekends the call must be placed after 8am. If you’re called during regular weekday hours you’d bill an emergency visit instead, which covers both the visit and the surcharge.
After 45 minutes, if you’re still at the hospital and you continue to treat patients you can add the continuing care premium to your claim. You can bill non-operative continuing care surcharges (billing items 01205, 01206, 01207) for each half-hour of care provided, as long as the criteria for those fees are met.
Remember though, if you’re scheduled to be there then you aren’t eligible to bill it on routine visits or rounds.
When adding the continuing care premium to your claim make sure you leave a note with ‘CCFPP’ (Continuing Care From Previous Patient) to show that you did not leave between patients. Without this note, you’ll be deducted 30 minutes from your claim (which may be the entire time you spent with your patient). Just a reminder for those being with us, our software will automatically add this note for you.
Timing for the the continuing care premium is based on the total time spent providing continuous care, not the number of patients you see. For example, if you see 3 patients within 30 minutes then you would only add the continuing care premium on the last patient, but for the entire 30-minute duration.
Tip: continuing care will not be paid until your Call Out premium is paid – which means if you have any issues with your call out claim, any subsequent continuing care will be refused. Always double check your call out claim is correct and isn’t missing a referring physician, start and end times, etc.
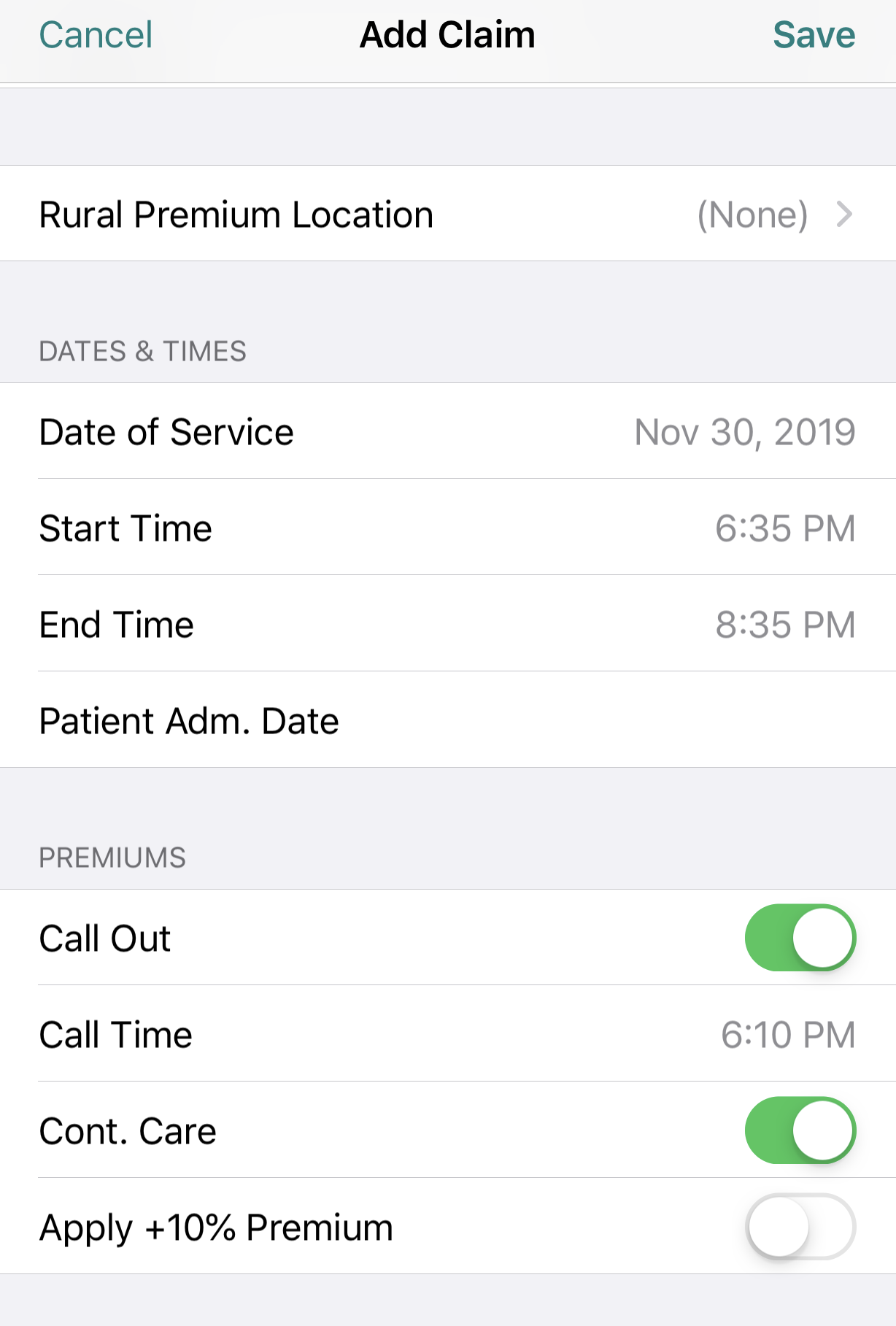
To apply these surcharges on Dr.Bill, log your consult or visit with the patient. On that claim toggle ‘Call Out & Continuing Care’. Don’t forget to enter the Call Time, Start Time & End Time for your encounter. Our app will automatically apply the correct Out of Office premiums to your claim.
2. Billing a Procedure with a Visit on the Same Day
When billing a procedure with a visit – on the same day – then visits should have a different diagnostic code than the procedure (if relevant). If the procedure and the visit have the same Diagnostic code then only one will be paid.
Medical billing in BC is confusing and can often be overwhelming. To help out, check out our complete MSP guide that walks you through each step of medical billing – from the general teleplan process to maximizing your claims and using mobile billing.
3. Billing a Consult with Multiple Visits
When billing a consult with multiple visits make sure you add the times of the consult and the visits. Independently this is not required, but when billed together it needs to be included so that MSP knows that the visits occurred at different times. Don’t forget to leave a note for multiple visits on the same day too (otherwise MSP will think it’s a duplicate claim).
Besides that, watch out for these 2 consult/visit mistakes we see often:
- Don’t bill more than 2 Directive care codes in a week – payments for directive care are limited to two visits per patient per week (Sunday to Saturday), even when there is no interval between visits.
- Don’t log ‘out of office premiums’ on Emergency visits – as these fee codes are designed to include your call out and thus are already included in the fee.Note: If you try to do this on Dr.Bill a warning pops up to try and prevent you from making this mistake!
4. Teleconferencing out of Province
Only 10001 (Urgent specialist advice – phone or in person) is covered through the reciprocal billing program. Other than that, if you’re conferencing on a patient who has health coverage outside of BC then you’re not eligible to bill teleconferencing fees.
5. Don’t Forget to Bill for Follow-Ups
If you’re following up on a patient don’t forget to bill for it. For example, if you’re a GP calling the hospital, you can bill 14077, a patient conference fee, that pays $40 per 15 minutes.
(MSP has various conference calls/follow up fee codes for most specialties).
6. Billing for Newborns
Newborns are billable under their mom’s PHN for the first 3 months while they wait until their own PHN is registered with MSP. For example, if born Feb.18th then you can bill them under their mom until April. However, after 3 months remember to bill them under their own PHN otherwise your claim will come back rejected.
7. The Difference between a Limited Consult vs. a Full Consult
A limited consultation requires all of the same components expected of a full consultation (within your specific specialty) but is less demanding and normally requires a lot less of your time than a full consultation.
Typically a full consultation is only payable once per patient every 6 months. There are also some specialties that allow a new consultation per admission (e.g. Internal Medicine Complex Patient). Whereas sometimes, you only need to provide an explanation in the notes field of the claim to let MSP know the medical necessity for the consultation within the 6 month period.
There’s no limit to how often you can log a limited consult. That being said, in our experience, MSP tends to reject limited consults if its been previously logged within the last 42 days.
Generally, a limited consultation, when medically necessary or specifically requested, will be billed as part of continuing care, and a full consultation is billed for a new/complex consultation.
8. Writing off Claims
A write off should only be done when you are eligible for the claim but due to circumstances such as invalid patient insurance, you cannot recover payment. This would qualify as a true write off that you can use for tax purposes.
Any other claims that are just refused because they didn’t meet MSP’s criteria should be cancelled instead as they do not qualify as a tax write-off.
9. Avoid Overage Claims
Submitting your claims to MSP on time is very important to ensure you get paid for the services you provide. The deadline to submit claims to MSP is quite strict. Follow our tips to avoid lost income:
- The MSP deadline is 90 days from the date of service. We suggest submitting within 75-80 days. This helps account for transmission time, number of days in a month, and any pre-edit refusals. That way, if there’s an error or a problem with your claim, you’ll still have time to resubmit it before the deadline.
- If a claim gets refused immediately by the MSP system (pre-edit refusal), then it has not officially been submitted. You’ll need to fix the reason for the refusal and resubmit it.
- If you’re billing with Dr.Bill check the web version of your account for any refusals. These will be called “submission errors”. We automatically correct and resubmit any refused claim, but we may need more information from you. In that case there will be a notification under Billing Issues (at the top right of your dashboard).
- If claims are <
strong>not submitted within the 90-day deadline, they will come back as a BV refused claim. At that point we can help you send in an ‘over-age claim request’ in an attempt to recover it. If this is the case, reach out to us and we’ll be able to provide you with more details.
10. Avoid these Common Rejections
There are certain mistakes we always see – a lot of which can be avoided. The following 5 items are the most common reasons for MSP rejections:
- The location of fee code doesn’t match.For example, a radiologic fee code performed in the ER.
- There’s a fee code conflict – so assessment is required.For example, maybe you picked a fee code that’s not eligible within your specialty. Or, maybe you selected a diagnosis that is not within the list of required diagnostic codes for that fee code.
- Invalid use of Premiums.For example using the continuing care premium when you’re not called into the hospital. Or logging ‘out of office premiums’ on emergency visit fee codes.
- There’s no referring physician.Most MSP claims for consultations (and some visits) require a referring physician. If you forget to add this then your claim will bounce back and you’ll need to fix it then resubmit it. While this is an easy fix, it will delay your pay for that claim so always double-check this before submitting.
- Your patient doesn’t have insurance.MSP will reject your claim if your patient doesn’t have valid health insurance (or if they have insurance from Quebec) as your claim isn’t eligible for reimbursement.If this is the case, you can send your patient a private invoice. For example, if you’re billing with Dr.Bill, you would send a private invoice the exact same way you submit an MSP claim, except, on the patient’s profile select ‘private’ instead of ‘public’.It’s also important to note that every Monday we run eligibility checks on previously refused claims, due to inactive MSP coverage, and anything that now has coverage, is automatically resubmitted to MSP.
Most rejected claims are a direct result of either not adding a referring physician OR not double-checking that your patient has insurance. So, make sure you always check these two things before submitting a claim.
Our last bit of advice…
When you do get a MSP error it will be accompanied by a code. This code lets you know what went wrong with the claim so you know how to fix it.
MSP List of Explanatory Codes
It’s always a good idea to keep track of your rejections and make sure you’re re-submitting them so that you don’t miss out on lost income.
Remember that on most of our plans we handle all your MSP rejections for you. This saves you time and headaches. So far, we’ve recovered funds for over 10,500 claims that might have otherwise gone unnoticed or sat as refused.
If you’re getting a rejection that wasn’t mentioned here, or have a question about a specific fee code, reach out to our billing team and we’ll be happy to help.

Download the new eBook
Our eBook can help you learn where to find locum jobs, what compensation to expect, which contract points may be up for negotiation and how to bill for your services.






