If you’ve received a rejection or refusal for one of your OHIP claims, you’re not alone – many doctors, especially those who are new to clinical practice, can make the kind of billing mistakes that lead to a claim not being approved. While many of these billing mistakes are easy to fix and resubmit, others are more complex. The good news is that plenty of doctors have been in your shoes! Here are some examples of claim rejection and refusals, and some tips for how to fix them:
Rejection: Billing C124 and E083 before 48 hours
Fee code C124 (‘subsequent visit by the Most Responsible Physician – day of discharge’) can only be billed if your patient has been in the hospital for two full days since their first hospital admission assessment and is discharged on or after day 3. If you bill C124 and your patient is discharged before this point, your claim will be rejected.
To fix the problem, you can use fee codes C122 (‘subsequent visit by the most responsible physician – day following the hospital admission assessment’) and C123 (‘subsequent visit by the most responsible physician – second day following the hospital assessment’) combined with Subsequent visit by the mrp premiumE083. If your patient is discharged on the first day after their hospital admission assessment, use C122 with E083. If your patient is discharged on the second day after their assessment, use C123 with E083. All of these codes will pay you the same amount, but selecting the right one will make sure your claim is approved.
Refusal: Unacceptable Diagnostic Code
While refusals from OHIP are usually easier to fix than rejections, they can still be inconvenient. One example of a rejection is when the diagnostic code you’ve chosen isn’t specific enough for the fee code you’re trying to claim. Make sure to use the correct 3 digit number for the diagnosis or your OHIP claim will come back rejected.
For example, in a patient with a strained elbow, you might look at the diagnostic codes in the OHIP schedule of benefits and choose code 840 (‘Strains, sprains and other trauma, shoulder, upper arm’) or 842 (‘Strains, sprains and other trauma, wrist, hand, fingers’), thinking that they’re the most similar to the injury. However, since elbows are never mentioned in either of these codes directly, the code you should be using is 848 (other sprains and strains). It might seem small, but scenarios like this will lead to OHIP claims being refused.
Rejection: Billing Related OHIP Codes on Separate Claims
Codes that are related should always be billed on the same claim. If you bill a consultation plus a special visit premium, you need to ensure that everything is added on the same encounter or you’ll run into rejections. The same goes for ‘add on codes’ that are percentage based, which must be included in the same encounter as the main fee code. For example, C122 and E083 must always be billed together on the same encounter. Since E083 gives you an extra 30% on C122, billing it alone won’t work because it doesn’t have anything to calculate off of so will end up getting rejected.
In the web version of Dr.Bill, E083 will appear as an eligible code that can be clicked and quickly added to the claim.
Rejection or Refusal: Billing Special Visit Premiums with Counselling Codes
Since special visit premiums are used for unexpected travel and urgent/emergent situations and counselling appointments are technically pre-booked, special visit premiums will never apply. Claims with this problem can come back either refused or rejected, depending on the situation, but the solution is the same for both scenarios – just remove the premiums and resubmit.
Rejection: Billing Counselling Codes with an Assessment for the Same Diagnosis
Under OHIP’s guidelines you are allowed to bill counselling codes (like Counselling Code K013) and assessments on the same day. However, these codes need to be on separate claims and also need to have different, unrelated diagnostics. In other words, you are able to bill a counselling code and an assessment code on the same day, but only if you include it in two separate claims, for two different issues.
Refusal: Missing or Incorrect Admission Date
C codes for inpatients must have an admission date or they will be rejected. The same goes for billing an admissions assessment – if the admissions date doesn’t match the date on the admissions assessment, it will be rejected. OHIP claims will commonly get refused for any type of mismatch between the fee code you use and the other information you’ve entered for the claim, so this is one place you should always double check.
Refusal: No Patient Insurance
If your claim is refused because your patient doesn’t have coverage under OHIP, you have two options – if the patient truly has no insurance, you’ll need to send them a private invoice. If you think you got the patient information wrong (for example, an incorrect version code or OHIP number) then you should call for verification – if you have a Comprehensive Plan with Dr.Bill, we handle this part for you.
Rejections you Can’t Recover
While many of the rejections described above are easy to fix, there are some situations when your claim can’t be recovered. Here are a few things to note:
Claim Paid to Another Physician
If the same claim was paid to another physician – including an identical patient number, fee code, etc. – then you probably won’t be eligible for reimbursement. However, it might be possible to claim a lesser code for the visit. For example, if the other physician billed C122 and special visit premium E083, you can rebill C122 as a subsequent visit without the premium.
Second Rejections
If you’ve resubmitted a claim with an explanation and it still got rejected by OHIP, the claim is no longer recoverable. This is a great example of why you should always double check your billings before submitting!
Exceeding the Claim Limit
Some fee codes come with their own set of rules about how often they can be used and when. For example, subsequent visit C002 (‘subsequent visits – first 5 weeks’)
is only allowed once a day for the first 5 weeks. After that point you can use C007 (‘subsequent visits – sixth to thirteenth week’) 3 times per week from week 6 through 13, and C009 (‘subsequent visits – after thirteenth week’) 9 times per month afterwards. Make sure you know each code’s limit before trying to resubmit.
Double Billing (Service Included in Previously Paid Item)
In some cases, the service you are trying to claim may be included in another paid item. For example, the critical care codes G400 (‘Critical care diagnostic & therapeutic procedures’) and G401 (‘Critical care diagnostic & therapeutic procedures – 2nd to 30th day’) cannot be billed with counselling codes, because counselling is included as a service in both G400 and G401. If you tried, your counselling codes would end up being rejected since technically you’re already being paid for them if you submit a critical care code.
OHIP Explanatory Codes
If you’re a new doctor, you can expect a learning curve with OHIP billing and your fair share of rejections or refusals. Mistakes happen, but don’t be discouraged – when you do get an error, it will be accompanied by a code and explanation, which you can then look up in our searchable database. The more you learn about why your claim was rejected or refused, the more likely you are to prevent it from happening again in the future.
This article offers general information only and is not intended as legal, financial or other professional advice. A professional advisor should be consulted regarding your specific situation. While information presented is believed to be factual and current, its accuracy is not guaranteed and it should not be regarded as a complete analysis of the subjects discussed. All expressions of opinion reflect the judgment of the author(s) as of the date of publication and are subject to change. No endorsement of any third parties or their advice, opinions, information, products or services is expressly given or implied by RBC Ventures Inc. or its affiliates.
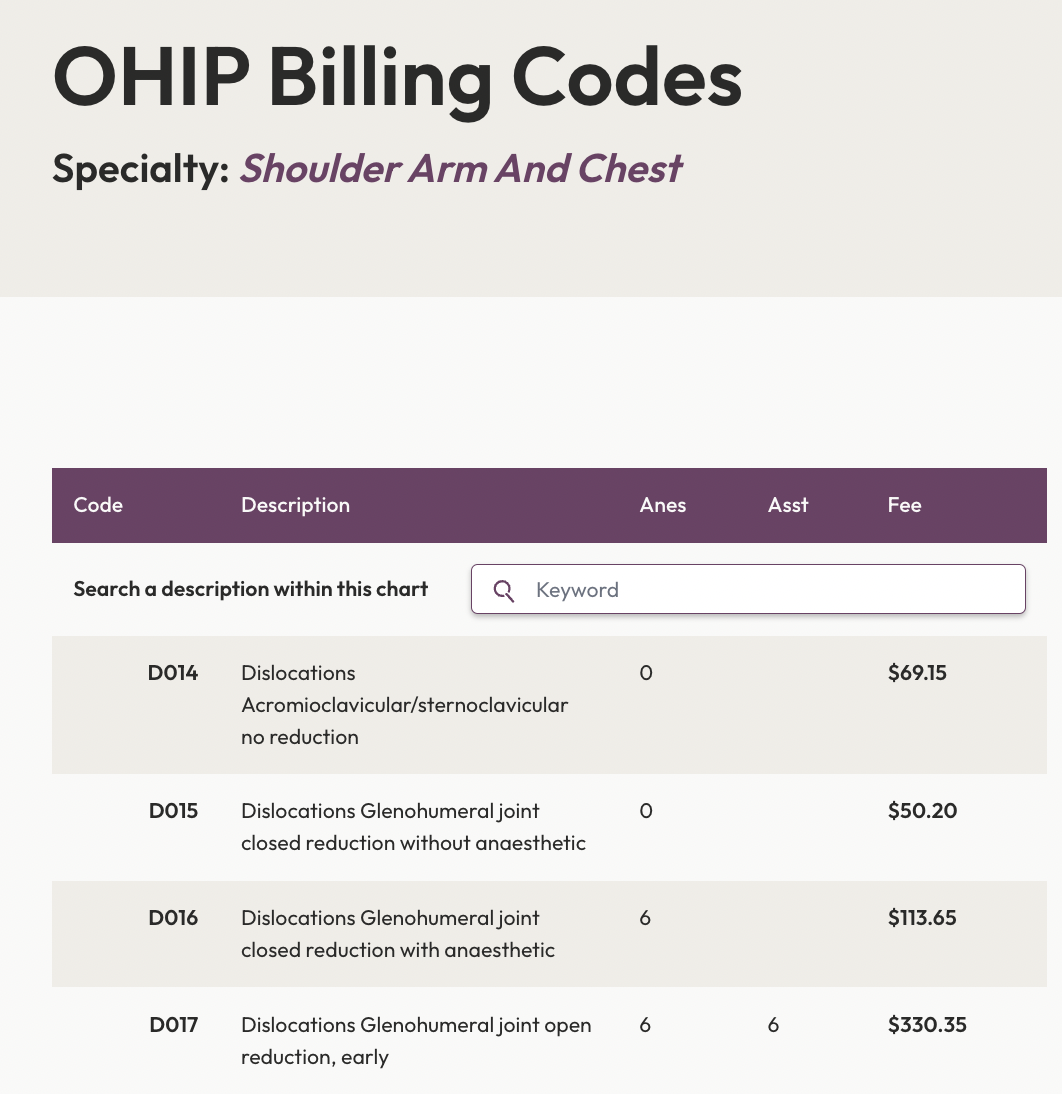
Search All OHIP Billing Codes
Search the Ontario Schedule of Medical Benefits electronically. We’ve digitized all the OHIP billing codes so you can easily find the most up to date billing rules and amounts.