The General Preamble is part of the BC Payment Schedule (often referred to as just ‘the schedule’) which lists all medical billing services that MSP insures, and how much each service pays.
Specifically, the General Preamble outlines the guidelines and billing rules under which certain fees are to be claimed. These rules act as a roadmap to understanding the schedule and as a summary of what is appropriate, and what isn’t appropriate, to bill.
In the schedule, MSP states that ‘fees cannot be correctly interpreted without reference to the general preamble.” Unfortunately, the general preamble is long and isn’t an easy read. In our experience, certain sections generate more questions than answers.
In order to navigate the MSP general preamble and payment schedule easier, use this mini guide to find exactly what resource you’re looking for.
The General Preamble and Payment Schedule Resources:
- The General Preamble and Payment Schedule 2019: Searchable Database
- MSP Billing Codes by Specialty
- The General Preamble PDF
- MSP Diagnostic Codes
- Remittance Advice Reports
- MSP updates
The General Preamble and Payment Schedule 2019: Searchable Database
An easier way to access BC medical billing fee codes and their rules, especially on a daily basis, is by using our searchable database.
This is an electronic version that outlines each fee code, its rules and prices. You can search by keyword, fee code or specialty.
MSP Billing Codes by Specialty
Opioid agonist treatment (oat)
Physical medicine and rehabilitation
Medical assistance in dying (maid)
The General Preamble PDF
The general preamble aims to clarify the rules of MSP fee codes so that you know exactly when you can, and cannot, use them. If you’re referencing fee codes daily, we suggest using the searchable database, however, if you’re a new physician, or new to BC, then it’s best to read over the general preamble and the payment schedule at least once. This will help you get a better understanding of the terminology MSP uses, as well as create a good foundation for what’s billabl
e.
However, keep in mind, if there’s something outlined in the general preamble that conflicts with a fee code or something outlined in your specialty’s section of the schedule, then the specialty rule triumphs it.
The general preamble starts on page 1 of the 481-page pdf and goes until page 35. It outlines 4 sections of the schedule.
The first section of the general preamble is the introduction, which outlines the necessary requirements (unless otherwise stated in a specific section), that all fee codes must include in order to be claimed and paid.
The second section lists the definitions found throughout the schedule. These are things you’ll see in fee code descriptions and general MSP terminology. For example, age categories, diagnostic facilities, referrals, etc.
The fourth and fifth sections of the general preamble list all administrative items and their descriptions, as well as the different types of services. For example, telehealth, examinations, surgery, etc.
Medical billing in BC is confusing and can often be overwhelming. To help out, check out our complete MSP guide that walks you through each step of medical billing – from the general teleplan process to maximizing your claims and using mobile billing.
MSP Diagnostic Codes
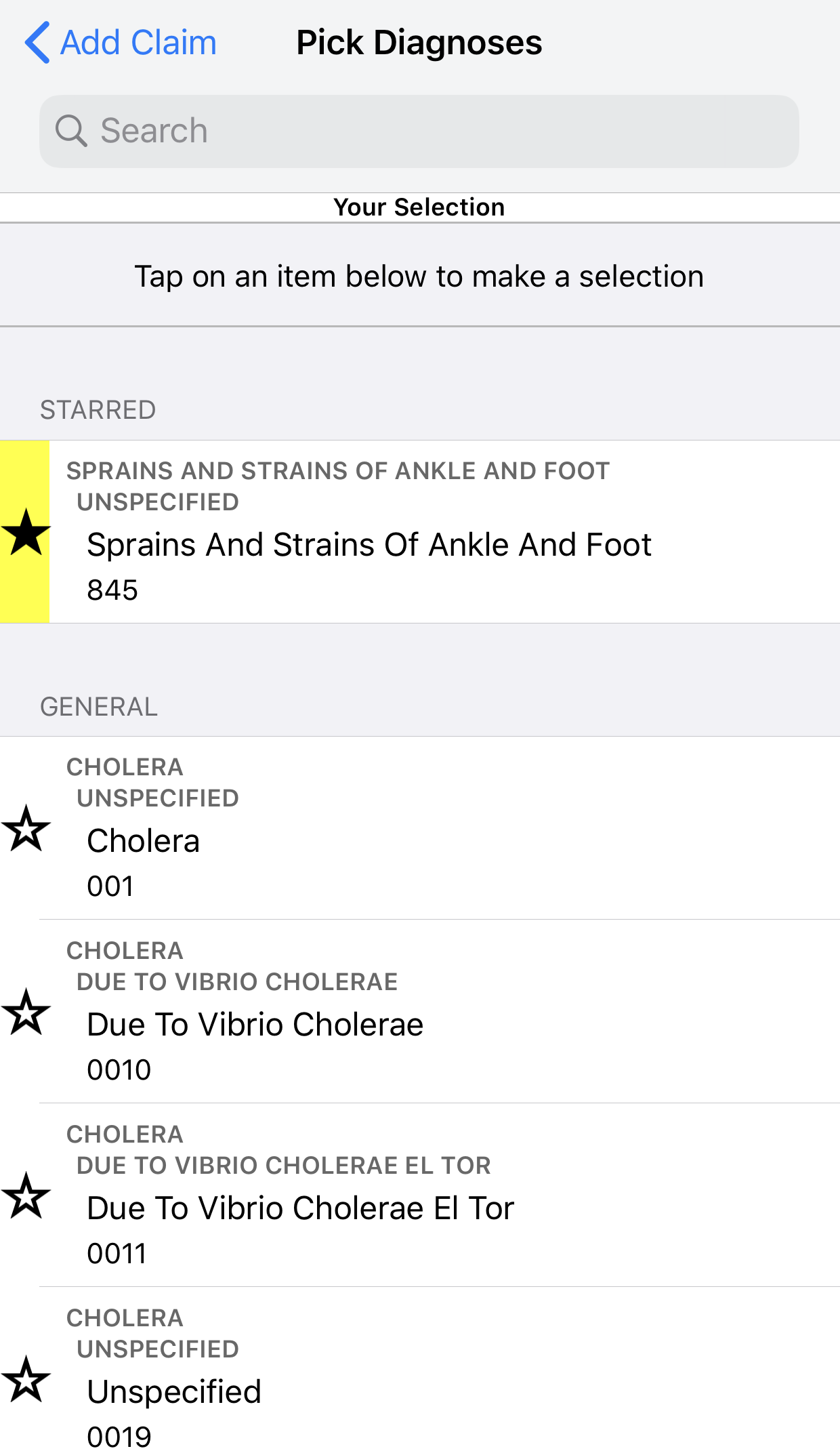
Any claim you submit to MSP must include a billing code along with a diagnosis. A diagnosis helps verify your claims, as well as generate statistics about illness and death.
If you’re submitting claims with Dr. Bill you can search for a diagnostic code directly on the app, just click on ‘diagnosis’ and search by keyword or code. If you’re always going to be using the same diagnostic codes you can tap the star icon to save it at the top of your list for easy searching. It’ll be saved for next time.
The diagnostic codes used by MSP are based on the ninth revision of the International Classification of Diseases, commonly referred to as ICD9, which were developed by the World Health Organization.
A List of MSP Diagnostic Codes
Index for 3 and 4 Digit Diagnostic Codes (ICD9)
Diagnostic Code by Section/Codes:
001 – 139.9: Infection and Parasitic Diseases
140 – 239.9: Neoplasms (PDF, 41KB)
240 – 279.9: Endocrine, Nutritional and Metabolic Diseases and Immunity Disorders (PDF, 19KB)
280 – 289.9: Diseases of Blood and Blood Forming Organs (PDF, 10KB)
290 – 319: Mental Disorders (PDF, 15KB)
320 – 389.9: Diseases of Nervous System and Sense Organs (PDF, 52KB)
390 – 459.9: Diseases of the Circulatory System (PDF, 23KB)
460 – 519.9: Diseases of the Respiratory System (PDF, 16KB)
520 – 579.9: Diseases of the Digestive System (PDF, 24KB)
580 – 629.9: Diseases of the Genitourinary System (PDF, 26KB)
630 – 676.9: Complications of Pregnancy, Childbirth and the Puerperium (PDF, 30KB)
680 – 709.9: Diseases of the Skin and Subcutaneous Tissue (PDF, 13KB)
710 – 739.9: Diseases of the Musculoskeletal System and Connective Tissue (PDF, 25KB)
740 – 759.9: Congenital Anomalies (PDF, 208KB)
760 – 779.9: Certain Conditions Originating in the Perinatal Period (PDF, 201KB)
780 – 799.9: Symptoms, Signs and Ill-defined Conditions (PDF, 209KB)
800 – 999.9: Injury and Poisoning (PDF, 1.2MB)
V01 – V82.9: Supplementary Factors Influencing Health Status and Contact with Health Services (PDF, 47KB)
Additional Diagnostic Codes (PDF, 9KB)
MSP Diagnostic Codes for GPs
Use our search tool to find the diagnostic code and description you’re looking for.
Remittance Advice Reports
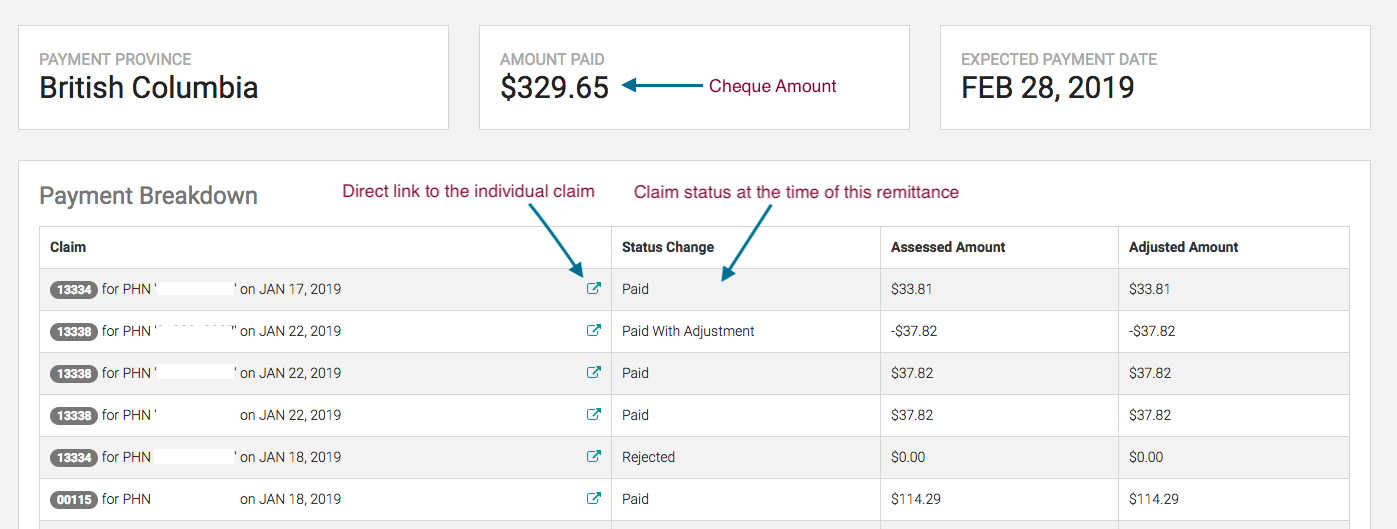
Typically 7-10 days after you submit your claims you’ll get a ‘MSP Remittance Advice (RA) Report’ and an ‘Error Code Report.’ These reports let you know which claims MSP has approved, paid with adjustment, rejected or have errors that you need to fix.
Remember from Chapter 1 of our Complete Guide to MSP Billing that your remittance report is provided through your billing program. What details you’ll actually be able to see also depend on the reporting capabilities of the billing software you’re using.
For example, at Dr. Bill, you’ll get daily reports along with your remittance report (twice monthly). Your reports allow you to:
- Easily see the status of each claim
- See a list of refusals
- See a list of rejected claims
- See which claims have been paid/paid with adjustment
Error Codes
Your reports might show that some claims have been rejected, reduced or refused.
If you do get an error, it will be accompanied by a code, and a description explaining what that code means. There are 706 possible reasons for this, which is overwhelming.
To make things easier, when you do get an error code, use our searchable database to figure out how to fix and resubmit it.
Explanatory Code Lookup
Payment Schedule (Cut-off dates)
MSP processes claim submissions in batches of 2 each month.
Imagine today is January 19th and it’s the deadline to submit your claims. You were last paid on the 13th, and the previous deadline was January 3rd.
All claims that you’ve submitted since the 3rd (up until 7pm today) will be processed for this cycle.
Use this payment schedule calendar to make sure you know when the next cut-off date is.
MSP Updates & Changes to the General Preamble
While there’s no set date or notification to when MSP updates the general preamble, it typically happens once or twice a year.
Between larger updates, you can expect MSP to release ‘broadcast messages,’ which are smaller updates on specific fee codes. These updates could be changes in the dollar amount that a particular fee code pays, the introduction of a new fee code or the removal of another one.
While these messages are short, they can sometimes be difficult to interpret. Chapter 5 of the MSP billing guide lists recent MSP broadcast messages in an easy to read to understand format, so you can stay up-to-date on these changes.
Dr. Bill Reminder:
If you’re billing with Dr. Bill, when MSP releases new fee codes, or adjustments, they are automatically updated and available both on the app and the web.
If you ever have a question about a rule, premium or fee code contact one of our MSP billing experts. They know the rules like the back of their hand, and can help you sort through anything!
This article offers general information only and is not intended as legal, financial or other professional advice. A professional advisor should be consulted regarding your specific situation. While information presented is believed to be factual and current, its accuracy is not guaranteed and it should not be regarded as a complete analysis of the subjects discussed. All expressions of opinion reflect the judgment of the author(s) as of the date of publication and are subject to change. No endorsement of any third parties or their advice, opinions, information, products or services is expressly given or implied by RBC Ventures Inc. or its affiliates.